
Nevertheless, descriptions for characteristic upbeat nystagmus and torsional nystagmus (with the top pole of rotation beating toward the affected ear), such as specific parameters of velocity, time course, and angle of positional nystagmus remain inadequate. However, there is still little evidence concerning the immediate correlation between nystagmus parameters in the Dix-Hallpike test (DHT) with CRP efficacy although, characteristic nystagmus provoked by DHT is essential for diagnosing psc-BPPV. In BPPV patients with cervical vestibular-evoked myogenic potential (cVEMP) or ocular VEMP (oVEMP) abnormalities, quality-of-life was reduced as compared to those without these abnormalities ( 15). Furthermore, abnormal vestibular evoked myogenic potentials (VEMPs), as neurophysiological parameters, showed a chronic and resistive BPPV prognosis ( 13), while vertigo occurring immediately after a maneuver as a liberator sign, correlated with the success of treatment ( 14). Other studies investigating the role of other prognostic factors, such as arteriosclerotic turn over ( 10), prior trauma or labyrinthitis ( 11), previous BPPV history, and intensity of nystagmus ( 12) predicted a low correlation for BPPV outcomes. However, other studies have shown a negative correlation between osteoporosis/vitamin D deficiency and BPPV ( 9). Moreover, some studies have concluded that patients with osteoporosis have a higher risk of occurrence and recurrence of BPPV ( 8). There have been studies investigating how osteoporosis may be a key predictor of BPPV prognosis ( 7). Therefore, developing a test or parameter that could predict the efficacy of CRP would profoundly contribute to a more reasonably distributed patient care. Furthermore, such symptomology may also leave patients, especially elderly patients, at a high-risk for catastrophic falls and a tremendous psychological burden ( 6). Although BPPV is a benign vertigo disease and is somewhat self-limiting, the onset of vertigo, vertigo-associated symptoms, and residual symptoms in resistant BPPV affects a patient's health and quality-of-life. Despite the success of the canalith repositioning procedure (CRP) in treating psc-BPPV, there remains 20% of the BPPV population that does not benefit from CRP ( 5). Moreover, due to differences in the anatomy of the semicircular canal, the posterior semicircular canal happens to be the most frequently involved canal in BPPV (i.e., psc-BPPV), which accounts for 85–95% of BPPV cases ( 4). The unilateral inner ear system contains three semicircular canals, including the anterior semicircular canal, horizontal semicircular canal, and posterior semicircular canal. BPPV accounts for nearly 30% of vertigo cases, with a lifetime prevalence of 2.4% in the general population ( 2, 3). Accepted for publication Jan 30, 2020.īenign paroxysmal positioning vertigo (BPPV) is defined as a disorder of the inner ear characterized by repeated episodes of positional vertigo ( 1). Keywords: Benign paroxysmal positioning vertigo (BPPV) posterior semicircular canal nystagmus repositioning maneuvers This association corresponded to the observation that psc-BPPV patients with a decreased time course and increased velocity in the slow phase of recording nystagmus have a worse prognosis of their BPPV persisting after a single CCRP. OR 2.96, P=0.035) remained an associated factor of maneuver resistance.Ĭonclusions: Decreased canalith weight on the affected side was associated with resistance to the CCRP. Moreover, an increased vertical velocity amplitude in the DHT during slow phase nystagmus (OR 3.16, P=0.029 vs. Results: With univariate and multivariate analysis, we observed a decrease in vertical time course during slow phase nystagmus on the affected side (odds ratio, OR 0.77, P=0.011 vs. Univariable and multivariable analyses were performed on age, gender, blood pressure, and nystagmus parameters of the affected side in the DHT in order to reveal associated factors causing resistance to the CCRP. Patients were retrospectively divided into two groups according to resistance to the CCRP.
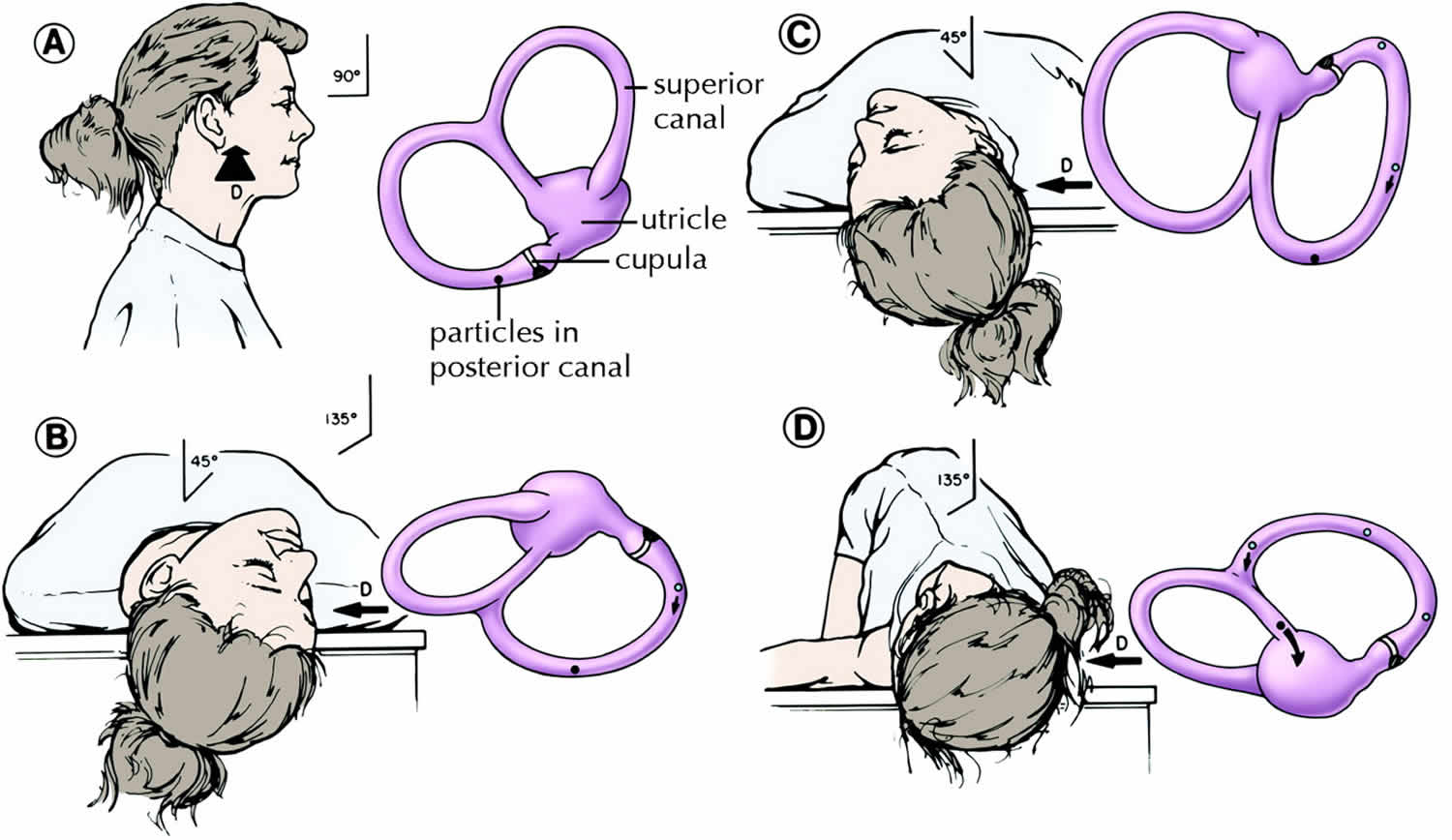
Additionally, positional nystagmus in the DHT was observed through a video-oculography. Methods: We reviewed 357 patients with unilateral psc-BPPV who underwent the computer-controlled canalith repositioning procedure (CCRP), which mimics the Epley maneuver. This study aimed to investigate the parameters of positional nystagmus in the DHT as prognostic factors for unilateral psc-BPPV. However, robust evidence regarding this diagnostic maneuver’s treatment efficacy is still lacking.

Policy of Dealing with Allegations of Research Misconductīackground: Nystagmus (i.e., involuntary eye movement) provoked by the Dix-Hallpike test (DHT) is considered the gold standard for diagnosing posterior semicircular canal benign paroxysmal positional vertigo (psc-BPPV).Policy of Screening for Plagiarism Process.
